Is Fibromyalgia Real? 10 Myths About Fibromyalgia and the Truths Behind Them
Those suffering from fibromyalgia often hear the question “Is fibromyalgia real?” Yes, Fibromyalgia is a complex and poorly understood condition characterized by tenderness and ongoing pain. Today, we’ll discuss 10 common myths about the condition, and the truths behind them.
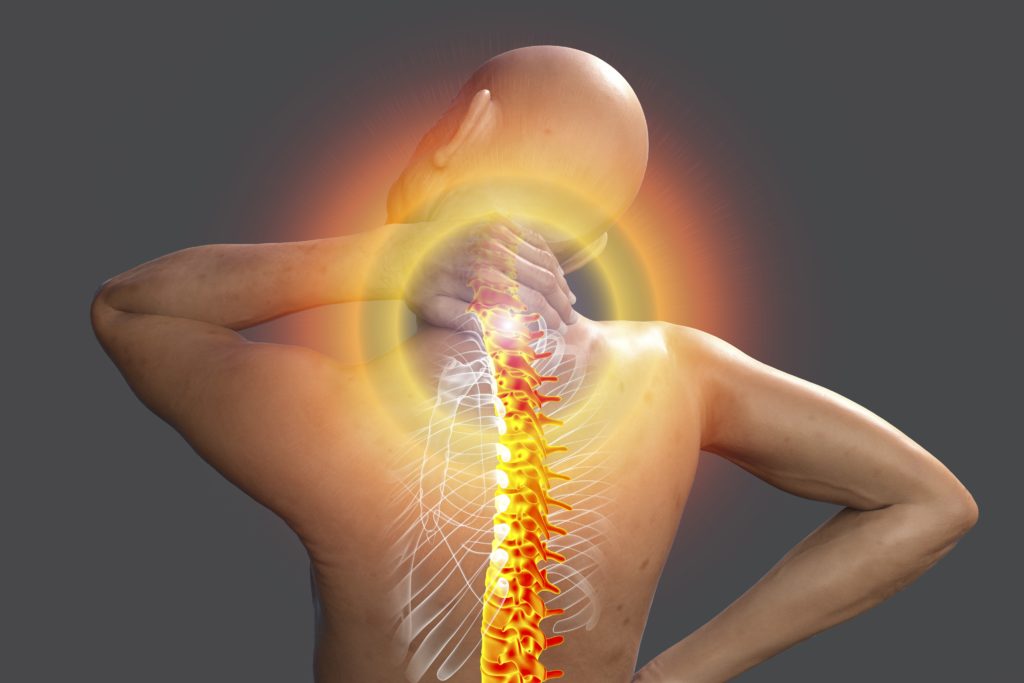
Fibromyalgia is a complex and poorly understood condition characterized by tenderness and ongoing pain in multiple areas accompanied by fatigue, restlessness, and brain fog for a period of at least three months.
For a patient to be diagnosed with fibromyalgia, other causes must be ruled out – including certain neuropathies, other physical conditions, viral infections, a different condition with similar symptoms, and more.
Fibromyalgia was only recognized by the WHO and added to the International Classification of Diseases as a health condition as recently as 1994, and there are still questions about how exactly to describe or diagnose the condition. While we know little about its mechanisms, we are aware of its prevalence and of certain treatments that are effective in the long term.
Common Misconceptions and Myths
However, as with any poorly understood health condition, there is a myriad of harmful myths and misconceptions surrounding fibromyalgia pain and the related diseases it may be conflated with. Understanding fibromyalgia can help you seek out proper treatment, as well as provide better support for any affected loved ones. Let us tackle and address a few common fibromyalgia myths.
1. “Fibromyalgia Isn’t Real”
One of the most common questions is, “is fibromyalgia real?”
In short, yes, fibromyalgia is real; however, the argument can be made that it is insufficiently understood. To this day, we do not have a consensus on its cause, or etiology, nor its pathophysiology, or the exact mechanism by which it occurs.
Current definitions for fibromyalgia rely on diagnostic criteria established and set forth by different medical organizations, such as the American College of Rheumatology, which offers guidelines for a clinical diagnosis that does not require physically testing tender areas for pain.
These diagnostic criteria ask patients to subjectively rate their fatigue levels, memory problems, and restlessness on a scale of 0 to 3, as well as confirm or deny the presence of depressive symptoms, headaches, and abdominal cramps, and specify areas they’ve experienced pain or tenderness in over the past week.
2. “It’s In Your Head”
Fibromyalgia is not classified as a mental health condition. It is not, in fact, all in the head – or psychosomatic, in other words.
While we aren’t sure how fibromyalgia develops, there is a difference between a fibromyalgia diagnosis and somatoform pain disorder, or the presence of pain that is completely devoid of any other physical symptoms and unexplainable by any underlying organic pathology. By current estimates, only about 60 to 80 percent of patients with diagnosed fibromyalgia would also fit the criteria for somatoform pain disorder.
By name, fibromyalgia is also defined as neurological pain in the nerves and muscles, and while its etiology is still being studied, we know it isn’t purely psychological.
3. “Fibromyalgia Is Like Arthritis”
Arthritis describes a number of different health conditions that affect the joints and cause joint pain, often in relation to an auto-immune disorder like rheumatoid arthritis.
While there are over a hundred different types of recognized arthritis, and both arthritis and fibromyalgia share symptoms of tender spots and consistent pain in multiple areas, fibromyalgia is not a type of arthritis.
4. “Fibromyalgia is Purely Physical”
Fibromyalgia is not purely psychological, but it is not purely physical either. There are psychological aspects crucial in the biopsychosocial model of fibromyalgia that helps effectively treat the condition.
What this means is that there are biological, psychological, and social (interpersonal) factors that affect and modulate the severity and onset of the condition.
5. “Fibromyalgia is Temporary”
While fibromyalgia can be managed and its symptoms can be successfully reduced, it is not a condition that comes and goes without proper intervention. Fibromyalgia is a chronic long-term condition that does not go away after onset.
6. “Fibromyalgia Always Requires a Special Diet”
There is no special diet that consistently reduces the symptoms of fibromyalgia. Good nutrition, meaning a balanced diet consisting of the macro and micronutrients the human body needs, will help a patient feel better if they haven’t been eating well. Other general health-conscious food guidelines, such as cutting back on alcohol, reducing daily caffeine consumption (especially afternoon), and reducing fried foods, can help improve general health as well.
But unnecessary dietary exclusions – such as cutting out all sugars, completely avoiding meat, or eating only meat – do not help improve symptoms.
7. “Only Medication Helps”
Pharmacology is not the only answer to fibromyalgia.
There are few medications that are well-tolerated and generally effective in treating fibromyalgia, outside of general analgesics such as NSAIDs and acetaminophen. The first-line treatments for fibromyalgia are physical activity, especially aerobic activity, and cognitive behavioral therapy.
Among medications, certain tricyclic antidepressants, monoamine oxidase inhibitors, selective serotonin reuptake inhibitors, and serotonin noradrenaline reuptake inhibitors may be used for the treatment of fibromyalgia although the FDA and European Medical Agency are split on which ones are approved. Only a few have been found to be efficacious, and the data is sparse.
8. “Movement Makes It Worse”
As mentioned earlier, physical activity is one of the most widely accepted and recommended treatments for fibromyalgia.
Not only does exercise trigger the release of endogenous endorphins and modulate pain, but aerobic exercise is also the only treatment that is strongly recommended by the European Alliance of Associations for Rheumatology.
9. “You Just Need Rest”
Fatigue and restlessness in fibromyalgia are not improved by sleeping more. Poor sleep quality is a common symptom of fibromyalgia, and for most patients, telling them to try and get more rest generally is not going to help. Stress modulation, a healthy diet, and exercise may help reduce symptoms, which in turn can lead to better sleep.
10. “Fibromyalgia Only Occurs in Older Women”
Studies among clinical populations show that women are eight times as likely to develop fibromyalgia versus men, but updated diagnostic criteria applied to epidemiology studies show a ratio closer to 2:1 female to male.
Prevalence for fibromyalgia in the general population sits at around 2 to 4 percent, and both children and adolescents can be diagnosed with juvenile fibromyalgia, though we aren’t sure how prevalent it is due to limited data.
Some researchers suggest that women were far more likely to be diagnosed with fibromyalgia in the past because they were more likely to describe an area as tender or painful during physical testing and because women generally consult healthcare professionals more frequently when experiencing somatic symptoms.
More recent criteria which do not require physically pressing on tender areas help reveal a much closer gap between male and female patients.
Treating Fibromyalgia Pain
Fibromyalgia is a difficult condition to be diagnosed with because it often describes the absence of symptoms that might define other similar pain conditions. However, fibromyalgia is far from untreatable. While it might not go away, symptoms can be reduced significantly through professional pain management and work with a specialized pain clinic.
Individual cognitive behavioral therapy, physical therapy, regular exercise, a sustainable healthy diet plan, and certain medication (if deemed necessary) can all help greatly improve quality of life and reduce symptoms.
Additional treatment options include:
Fibromyalgia is real. If you are suffering from pain, contact our pain management specialists today.
